Fentanyl Addiction, Withdrawal and Detox: Symptoms, Timeline & Treatment

Fentanyl is a powerful synthetic opioid that is driving a surge in overdose deaths across the U.S. Fentanyl addiction is becoming more widespread so understanding the symptoms, timeline and treatment options for withdrawal and detox is critical.
Detox is the essential first step in breaking free from fentanyl’s grip. This helps your body safely eliminate the drug while managing severe withdrawal symptoms. Effective treatment often begins with medically supervised fentanyl detox and continues with long-term support.
If you or someone you love is struggling with fentanyl then you can call now to find help. Early intervention can save lives and set the path toward lasting recovery. Let’s explore fentanyl, signs of addiction and how to get off fentanyl.
Recovery is possible — call today to find a fentanyl detox program that’s right for you.
What Is Fentanyl?
Fentanyl is a synthetic opioid that can be between 50 and 100 times more potent than morphine. Medically, it is prescribed to treat severe pain and is often prescribed for cancer patients or following significant surgery. Fentanyl must be prescribed under strict supervision and comes as patches, lozenges or injectable solutions.
However, illegally manufactured fentanyl is driving the opioid crisis. It might be combined with heroin, cocaine or counterfeit pills without your knowledge. This increases the risk of overdose from a highly potent drug.
Fentanyl side effects include drowsiness, confusion, slowed breathing and unconsciousness. In extreme cases, it may lead to what’s known as “fentanyl syndrome” which is a rapid overdose and respiratory failure. Understanding what fentanyl is and how it differs in medical vs street use is essential to addressing its deadly impact.
Fentanyl Side Effects and Risks
Fentanyl triggers serious short and long term side effects. Short term effects include extreme drowsiness, nausea, constipation, confusion and slowed breathing. Long term use may lead to tolerance, physical dependence and damage to your respiratory and cardiovascular systems.
One of the most harmful effects of fentanyl is its unpredictability. This is especially true when it’s mixed or “cut” with other substances like heroin, cocaine or counterfeit pills. These combinations dramatically increase your risk of overdose.
Fentanyl overdose symptoms include pinpoint pupils, cold or clammy skin, unconsciousness and slowed or stopped breathing. It’s so potent that even a tiny amount can be fatal. Understanding fentanyl side effects is crucial to preventing accidental overdose and death.
Signs of Fentanyl Addiction
Understanding how to quit fentanyl begins with recognizing the signs and symptoms of dependence and addiction. Fentanyl addiction can develop quickly because the drug is extremely potent. You can experience physical, psychological and behavioral fentanyl addiction symptoms.
Physical signs include drowsiness, constricted pupils, slowed breathing and frequent flu-like symptoms during withdrawal. Psychological symptoms manifest as anxiety, depression and obsessive thoughts about the next dose. Behavioral signs of fentanyl addiction feature secretive behavior, doctor shopping, isolation and neglecting responsibilities.
It’s important to distinguish between drug dependence and addiction. Dependence means you are physically reliant on fentanyl and experience withdrawal symptoms if you stop using it. Fentanyl addiction symptoms are characterized by compulsive use and behaviors despite experiencing negative consequences. The move from dependence to addiction happens quickly because of the drug’s strength and intensity.
Fentanyl Withdrawal: Symptoms and What to Expect
Fentanyl withdrawal is the process of eliminating the drug from your body after you’ve developed dependence or addiction. You can experience a range of physical and psychological symptoms as your body adjusts to functioning without it.
Don’t wait to get clean. Call today!
Withdrawal symptoms from fentanyl usually begin within 12 to 24 hours after you’ve taken the last dose and the duration and intensity will depend on several factors. For example, prescription fentanyl sometimes has a delayed and prolonged withdrawal process compared to the faster and more severe symptoms of illicit fentanyl.
High dose and long term users have more severe physical and psychological symptoms and people who use fentanyl with other drugs have a more complex withdrawal process. Fentanyl withdrawal can trigger complications that may be medically dangerous which is why a medically supervised fentanyl detox program is best.
Cravings are a common fentanyl withdrawal symptom. Other core symptoms include:
Physical
- Nausea
- Vomiting
- Diarrhea
- Muscle pain
- Sweating
- Chills
- Insomnia
- Anxiety
- Flu-like symptoms
- Pain
Psychological
- Mood swings
- Irritability
- Depression
- Panic
- Anxiety and agitation
- Cognitive disturbances
- Paranoia
These symptoms can easily lead to relapse without medical supervision. Withdrawing from fentanyl is challenging. Medically managed detox can ease symptoms and offer a safer path toward sustainable recovery.
Fentanyl Withdrawal Timeline
The fentanyl detox timeline depends on factors such as dosage, length of use, method of ingestion and co-occurring mental or physical health conditions. Symptoms will generally follow a predictable pattern. Here’s what to expect:
Early Symptoms 8–24 Hours: Withdrawal begins as the drug leaves the body. Common symptoms include anxiety, sweating, yawning, a runny nose and muscle aches.
Peak Withdrawal 36–72 Hours: This phase is usually the most intense one. You may experience severe nausea, vomiting, diarrhea, insomnia, chills and intense cravings. Medical support is often critical during this stage.
Symptoms Ease in Days 4–10: Physical symptoms gradually lessen but sleep problems, irritability and drug cravings typically continue.
Post Acute Withdrawal over Weeks to Months: Psychological and emotional symptoms may linger. Ongoing support is essential to remain in recovery.
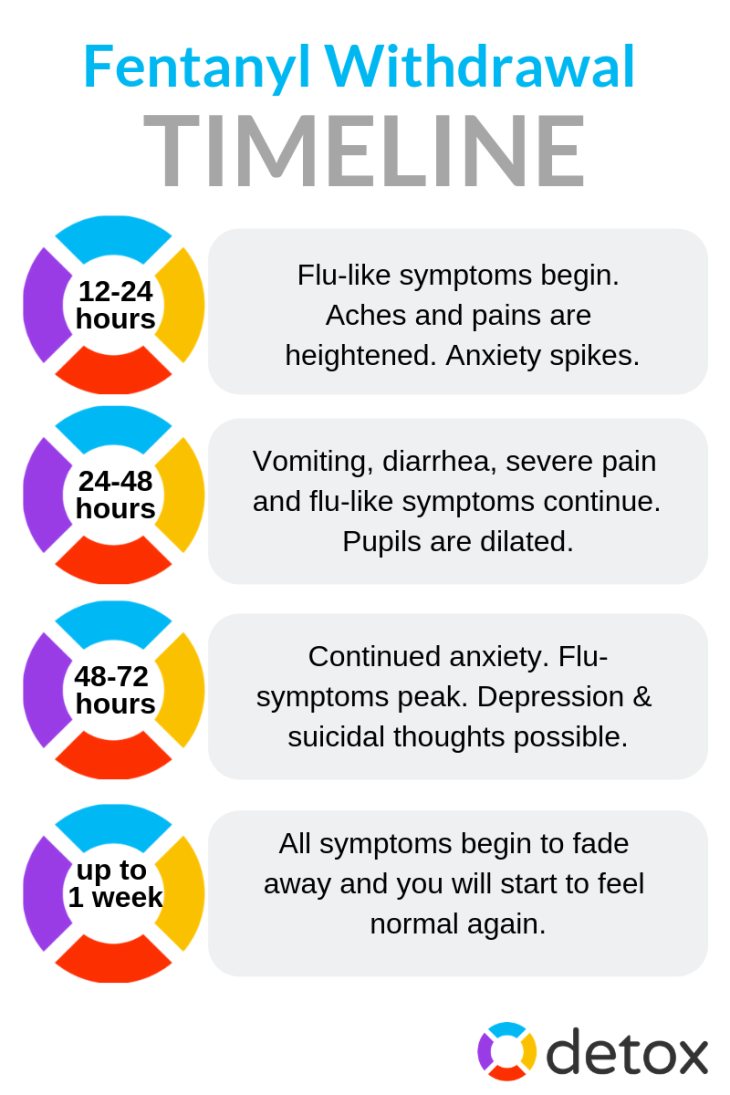
How long your fentanyl withdrawal lasts depends on the type of fentanyl used (prescription vs. illicit), the dosage and duration of use, your metabolism and whether medical support or tapering methods are used during detox. Illicit fentanyl is often stronger and faster-acting and it can cause more abrupt and severe withdrawal. Detox from prescription patches may be longer and slower.
Fentanyl Detox: What It Is and Why It Matters
Fentanyl detox is the medically supervised process of eliminating fentanyl from your body while managing withdrawal symptoms. The primary goals of fentanyl detox treatment are stabilization, safety and reducing physical and emotional discomfort.
A medical program is the best way to detox from fentanyl as it reduces the risk of relapse and life-threatening complications. Medical detox provides round the clock monitoring, medications to ease symptoms and immediate intervention if complications arise. Supervised fentanyl detox also serves as the first step in a longer recovery process and improves the likelihood of treatment success.
Treatment Options for Fentanyl Withdrawal
Fentanyl withdrawal treatment often begins with medically supervised detox, where providers manage symptoms and may prescribe medication like clonidine or lofexidine to reduce withdrawal symptoms and discomfort.
Medication-assisted treatment (MAT) may be started during or after the withdrawal period using FDA-approved medications like methadone, buprenorphine, or naltrexone. These prescription medications for fentanyl addiction fill several roles. They help to reduce cravings, stabilize brain chemistry, and prevent symptoms of withdrawal.
Treatment for fentanyl addiction can also include behavioral therapies such as cognitive behavioral therapy (CBT) and contingency management. These treatments address the psychological aspects of addiction and help you change harmful thought patterns and behaviors.
Inpatient and outpatient detox programs are both effective and depend on the severity of addiction and the level of medical care needed. Your program may also incorporate holistic or spiritual support such as meditation, yoga or faith based counseling to address emotional healing and promote long-term recovery.
Inpatient vs Outpatient Fentanyl Detox: Which Is Right for You?
Choosing between inpatient and outpatient fentanyl detox depends on the severity of dependence, medical needs and personal circumstances. Inpatient fentanyl detox offers 24/7 medical supervision and support.
This is ideal when you have high-dose use, long term dependence or co-occurring mental health conditions. It provides a controlled and supportive environment that reduces your risk of relapse during the most critical withdrawal stages.
During outpatient detox you live at home while attending scheduled treatment sessions. Your doctor may prescribe medications for you to take at home to ease withdrawal symptoms. This is more flexible and often less expensive but it may not provide enough support if you have a severe addiction. The risk of complications or relapse is higher without continuous care.
Use your favorite online search engine and enter keywords such as “fentanyl detox near me” or “fentanyl rehab near me.” This can help you locate a center that offers confidential assessments and the appropriate level of care. You can also search our extensive online database to find detox centers near you!
After Fentanyl Detox: What Comes Next?
Getting off fentanyl begins with medical detox to address physical withdrawal. The next step is a structured rehab program to target the psychological, emotional and behavioral aspects of addiction.
Start the first step of your recovery journey. Call Today.
In fentanyl rehab, you can expect personalized counseling, evidence-based therapies like cognitive behavioral therapy (CBT) and group sessions that build community and accountability. Relapse prevention strategies are a core focus and help you identify triggers and create healthy coping skills.
Rehab may also offer life skills training, family therapy and dual diagnosis support. Ongoing aftercare such as outpatient therapy, peer support groups and sober living helps maintain progress. Your long term recovery is more successful when supported by comprehensive therapy and treatment beyond detox.
How to Get Off Fentanyl Safely
Getting off fentanyl safely requires medical guidance and a personalized treatment plan. Using a “cold turkey” approach to getting off fentanyl at home can lead to severe withdrawal symptoms. These symptoms include vomiting, dehydration, and cravings which increase the risk of relapse or overdose.

A safer approach is tapering. The dosage is gradually reduced under medical supervision which eases symptoms and supports your body’s adjustment. For many people, the best way to get off fentanyl is through a medically supervised detox program.
Healthcare professionals monitor your symptoms and may use medications like buprenorphine or clonidine to reduce discomfort. However detox is only the first step. Treatment should include therapy, relapse prevention and ongoing support. Trying to get off fentanyl at home without supervision is risky and not recommended.
Start Your Journey to Recovery Today
Recovery from fentanyl addiction is possible and it begins with the decision to seek help. With medical support and a personalized treatment plan you can safely detox and take the first step toward a healthier, drug free life.
Professional care ensures your safety, eases withdrawal symptoms and connects you to long-term support through therapy and aftercare.
You don’t have to go through this process alone. Help is available every step of the way. If you or someone you love is struggling with fentanyl then call now or use our online tool to search for a fentanyl detox center near you. Healing starts with one brave choice.
Fentanyl Detox FAQ
Can You Detox From Fentanyl at Home?
Detoxing from fentanyl at home is dangerous and not recommended for some people because of the risk of severe withdrawal symptoms including intense cravings, vomiting and life-threatening complications. Medical supervision ensures your safety and comfort while providing proper physical and mental support. Always seek help from a licensed doctor or detox or addiction treatment center.
Fentanyl usually stays in your system for eight to 24 hours. Traces can be detected much longer. It can appear in your urine for several weeks, blood for 12 hours and hair for up to 90 days, depending on how much you use and your metabolism.
Yes, fentanyl withdrawal can be dangerous. Symptoms like severe anxiety, vomiting, muscle pain and insomnia can lead to dehydration or relapse. Sudden withdrawal without medical help increases these risks. Medically supervised detox ensures you have access to medications and support that manage symptoms safely and reduce complications.
The best way to treat fentanyl addiction is through a comprehensive, medically supervised program that combines detox, medication-assisted treatment (MAT), behavioral therapy and ongoing support. A medication detox program uses FDA-approved prescriptions like clonidine or buprenorphine to ease withdrawal and reduce cravings. This is most effective when combined with counseling to address underlying issues and promote long-term recovery.


